1. Dates
Dates are a traditional food in a lot of the world and are a good source of carbohydrates, B-vitamins, calcium, magnesium, potassium, fat, salts, proteins, and vitamins.
Research on dates related to childbirth isn’t about inducing labour specifically, rather studies have looked at the impact of eating dates in the weeks leading up to their due date.
Researchers think dates may affect your oxytocin receptors (the hormone that causes your uterus to contract), helping your uterine muscles respond better to the oxytocin your body produces, resulting in more effective contractions (and who doesn’t want those?).
A large 2019 systematic review (meaning they looked at all the studies related to a subject) and meta-analysis (meaning they pooled a group of similar studies into 1 group of data to learn more) examined the potential connection between the consumption of date fruit on childbirth outcomes.1
The systematic review included 11 studies totalling 921 pregnant people (18-35 years old), who were 36-42 weeks pregnant between 2007 and 2017. Eight of the 11 studies from the systematic review were included in the meta-analysis. These were low-risk, singleton pregnancies in people without diabetes.
Participants consumed anywhere from 50 to 100 grams of dates for 10 to 28 days. More specifically, in most of the studies included in the review, participants consumed 6 to 8 dates daily (60 to 80 grams) starting at 36 to 38 weeks of pregnancy until the start of labour.
These studies found an association between date consumption and many birth outcomes:

Although no harmful effects were seen in the studies, it’s important to talk to your healthcare provider before eating all. the. dates. 🙂
While I love dates, and will happily consume them on their own, I know some people find that less than desirable (like my sister-in-law). While some stores will sell ‘fancy’ dates (i.e. rolled in coconut or cocoa), below are some other ways to enjoy dates.

2. Evening Primrose Oil
Evening primrose oil (EPO) is oil from seeds of the evening primrose plant. Researchers think the 7-10% of gamma linolenic acid in it is the active ingredient because it’s a precursor of prostaglandins E1 and E2 – which are the prostaglandins that help ripen the cervix in prep for labour.
The first randomized control trial investigating the effect of EPO on the cervix was published in 2019.2
This study had 86 first-time birthers pregnant with 1 baby randomly assigned to get EPO or a placebo (43 in each group) – neither the pregnant person nor doctor knew what they were getting.
Participants had no; chronic health conditions, prior C-section/uterine surgery, pregnancy complications, or use of other techniques to induce labour (sex, laxatives, herbal capsules).
People were given a 1000mg daily dose of EPO (or placebo) in soft vaginal capsule every night, and asked to remain lying down for 2 hours if able, starting from 38th week pregnancy until birth.
Researchers found the following:

There was no difference in active labour (6 to 10cm) or the 2nd stage of labour (pushing), the use of Pitocin to speed up labour, Apgar scores, the amount of Pitocin used after birth, or the rate of postpartum hemorrhage. No side effects were reported.
Authors concluded EPO can ripen the cervix of first-timers at term and could be an ‘effective, safe, affordable’ option that doesn’t require hospitalization, and that more studies are needed.
3. Breast Stimulation

Breast stimulation releases oxytocin, which can ripen the cervix and cause uterine contractions.
Interestingly, breast and nipple stimulation for labour induction has been in the medical literature since the 1700s!
The American College of Obstetricians and Gynecologists (ACOG) has described nipple stimulation or unilateral breast stimulation as a natural and inexpensive nonmedical method for inducing labour.3
A 2006 Cochrane review of 6 randomized controlled trials (719 people) looked at self-breast stimulation in low-risk groups as a non-medical way to induce cervical ripening and/or labour. It found that in those who already had a ripe cervix:4

Six of the 7 trials used hand massage, one used a breast pump, and all did one breast at a time.
Since that study was published, an additional trial was done in 2014.5 It randomly assigned 200 first-time low-risk pregnant people to do self-breast massage (or not) starting at 38 weeks.
Cervical ripeness (via Bishop’s score) was assessed at 38 and 39 weeks.
They found:
- The breast stimulation group had a significant change in cervical ripeness between 38 and 39 weeks (from 3.02 to 6.08 in the stimulation group vs. from 3.12 to 3.9 in the control group)
- Pregnancy was slightly but statistically significantly shorter in the stimulation group (39.2 weeks vs. 39.5 weeks)
- There were fewer C-sections in the stimulation group (8% vs. 20.4%)
- Other outcomes were similar (labour duration, hyperstimulation, meconium staining, postpartum hemorrhage, neonatal outcomes)
Don’t forget, ALL of these studies were in low-risk pregnancies and research looking at high-risk pregnancies is still needed. None of the participants involved had a prior Caesarean.
Always talk to your healthcare provider before trying natural induction techniques to make sure they make sense for your unique situation.
4. Acupuncture
I got acupuncture with my second and third pregnancies. When I was still pregnant with my second, as I reached my due date (after being about 1.5 weeks early with my first), I was feeling really ready to help things along. While I’ll never know if it helped or not, research has some info for us.
One 2018 study compared 112 people receiving acupuncture every other day (starting at 40 weeks 2 days) to 263 receiving routine care – and as you can see, it seemed to have had an impact:6
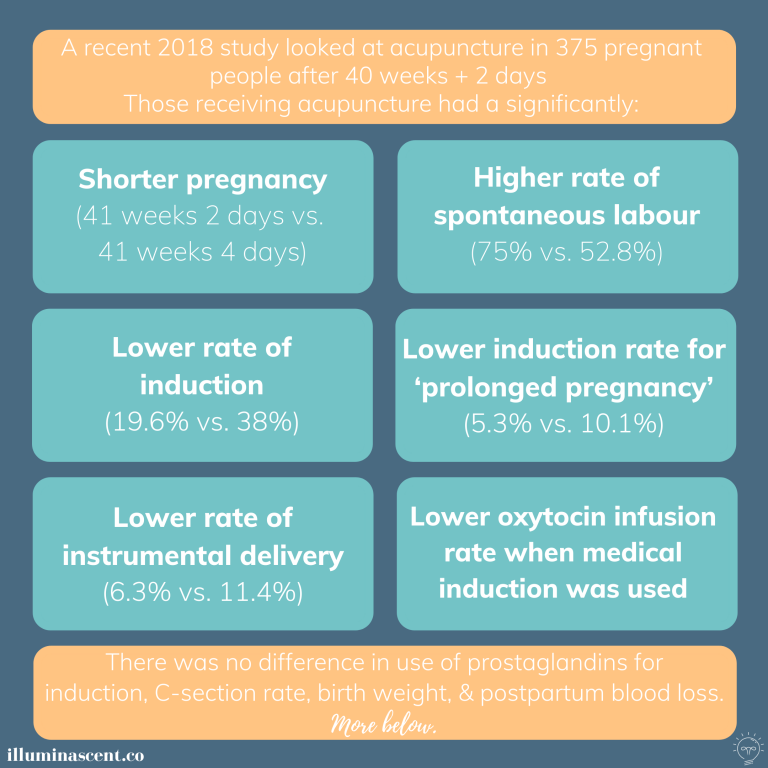
Additionally, before the above study was published, a large Cochrane review examined acupuncture in pregnancy (and thus didn’t include the above study).7
A Cochrane review (gold standard of reviews) looks at many studies on the same topic – with this one including 22 trials and 3456 people.
When looking at studies comparing acupuncture to sham control (i.e. pretend acupuncture), it reported:
- More cervical readiness for labour (as measured using Bishop’s score)
- No difference in C-sections between groups (8 trials, 789 people)
However, it did find that electro-acupuncture may be more effective than manual for outcomes of C-sections and instrumental vaginal and spontaneous birth. It reported:
- Decreased rate of C-section – 3 trials, 327 people
- Increased rate of spontaneous vaginal birth – 1 trial, 72 people
- Increased rate of instrumental vaginal birth – 2 trials, 271 people
Overall, there were no differences in oxytocin augmentation, epidural use, Apgar scores at 5 minutes, NICU admission, maternal infection, and maternal bleeding.
5. Castor Oil
Even though with 2 of my 3 pregnancies I was desperate for labour to just start, I always viewed castor oil (CO) as one of those mysterious ‘last resort’ kind of tactics.
Turns out, there’s been a lot of research on the topic.
Reports of CO to stimulate labour date back to ancient Egypt. A 2010 study exposing pieces of uterine tissue from a pregnant human to CO found the tissue exposed to CO had increased contractile activity vs. tissue just exposed to a salt solution.8
As always, don’t just go chugging CO! Talk to your care provider (some will be more familiar with this than others). Make sure it’s safe for your unique situation.
Here’s what 4 studies have found. All used one 60mL dose, & people were low-risk & 40-42 weeks pregnant. There’s no data in those with prior Caesareans.

Study 1:9
- 100 pregnant participants (randomly assigned to take CO or nothing)
- Those in the CO group had an increased chance of starting labour w/in 24 hrs vs. those with no treatment (58% vs. 4%)
- 100% experienced nausea in CO group, vs. 0% in the other
Study 2:10
- 43 pregnant people (randomly assigned to take CO or nothing)
- The CO group had a greater chance of starting labour w/in 24 hrs vs. those with no treatment (54% vs. 4%)
- CO group had a more ripe cervix
Study 3:11
- 80 pregnant people (CO vs. placebo of sunflower oil)
- Odds of being in active labour w/in 12 hrs was 3x higher with CO vs. sunflower oil
Study 4:12
- Review combined 8 studies
- CO more than 3x more likely to go into labour w/in 24 hrs
- No differences in C-section, forcep use, episiotomy, hemorrhage, meconium-stained amniotic fluid, NICU admissions, maternal death, stillbirth, uterine rupture
What's the take-home message?
- There are a variety of techniques that may help initiate labour in low-risk pregnancies
- Date consumption in the weeks leading up to childbirth is associated with a shorter pregnancy, faster labour, increased cervical dilation at admission, and fewer cases of using medication to start and speed up labour, vacuum assisted delivery, postpartum bleeding, and more
- Authors concluded EPO can ripen the cervix of first-timers at term and could be an ‘effective, safe, affordable’ option that doesn’t require hospitalization, and that more studies are needed
- The ACOG as has described nipple stimulation or unilateral breast stimulation as a natural and inexpensive nonmedical method for inducing labour. In those with a ripe cervix, more people go into labour within 72 hours following breast stimulation vs. those who don’t, and there’s also a major decrease in the risk of post-partum hemorrhage
- Acupuncture may result in a shorter pregnancy, lower induction rate, lower rate of instrumental delivery, and more
- Castor oil ingestion between 40 and 42 weeks (in low-risk pregnancies, no prior C-section or uterine surgery) may increase the chances of going into labour within 24 hours (with the side effect of nausea)
- As all of this research was conducted in low-risk pregnancies, more research is needed in higher-risk populations and in those with a prior C-section
- No safety concerns were associated with any of the above methods, though castor oil consistently caused nausea
- You should always talk to your care provider before using any of the techniques to ensure they are safe for your specific circumstances
References: 1. Nasiri M, et al. Complement Ther Med. 2019;45:71-84; 2. Najafi, M, et al. NPT. 2019;6(4):202-211; 3. Induction of labor. ACOG Practice Bulletin No. 107. Obstet Gynecol. 2009;114:386-97; 4. Kavanagh J, et al. Cochrane Database Syst Rev. 2005;3:CD003392; 5. Singh N, et al. Biomed Res Int. 2014;2014:695037; 6. Neri I, et al. J Acupunct Meridian Stud. 2018;11(5):332-336; 7. Smith CA, et al. Cochrane Database Syst Rev. 2017;10(10):CD002962; 8. O’Sullivan MD, et al. Am J Obstet Gynecol. 2010;202(5):453.e1-453.e4534; 9. Garry D, et al. Altern Ther Health Med. 2000;6(1):77-79; 10. Azhari S, et al. Saudi Med J. 2006;27(7):1011-1014; 11. Gilad R, et al. American Journal of Obstetrics and Gynecology. 2012;206:S77-S78; 12. Zamawe C, et al. BMJ Open. 2018;8(10):e022499. Published 2018 Oct 17.

